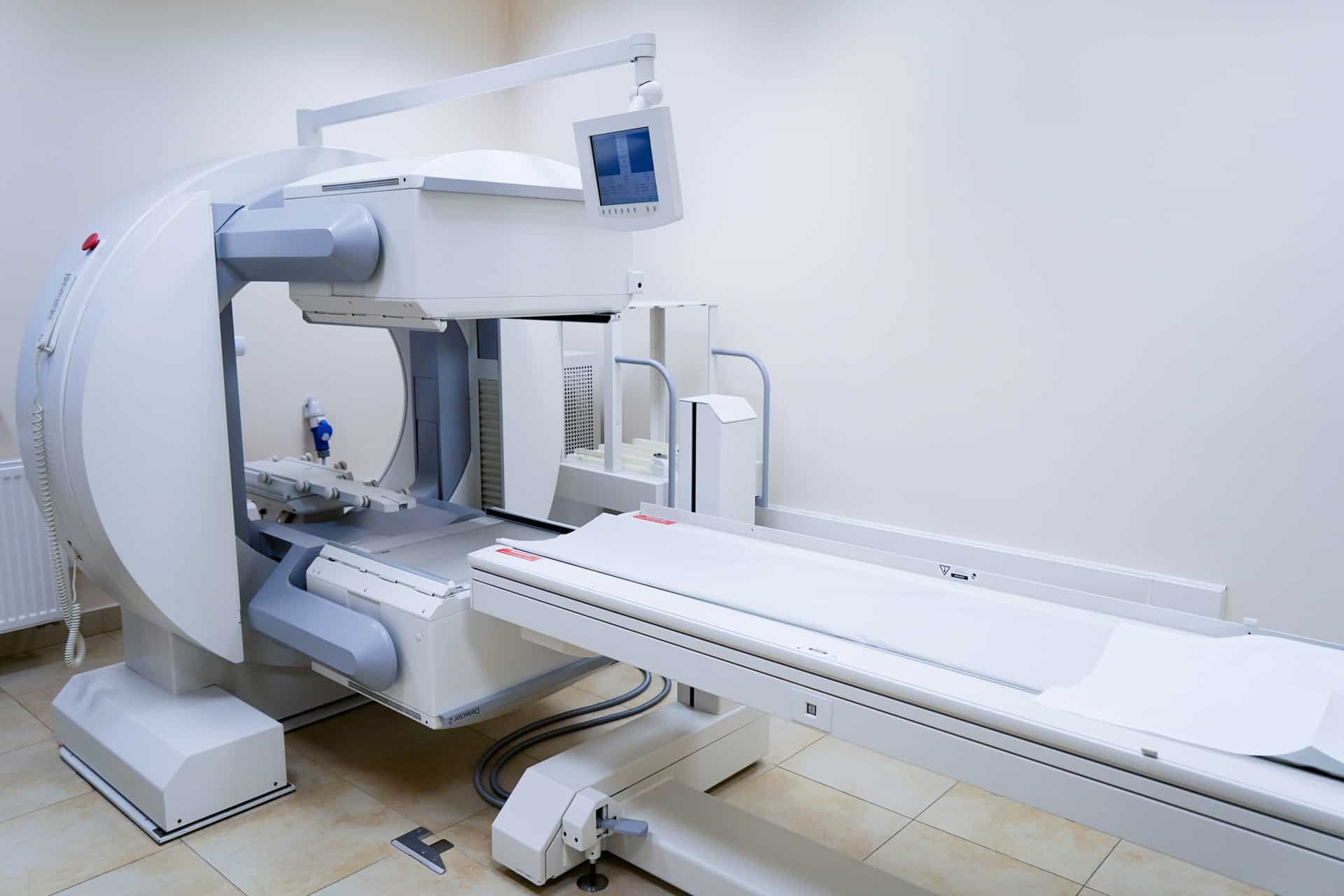
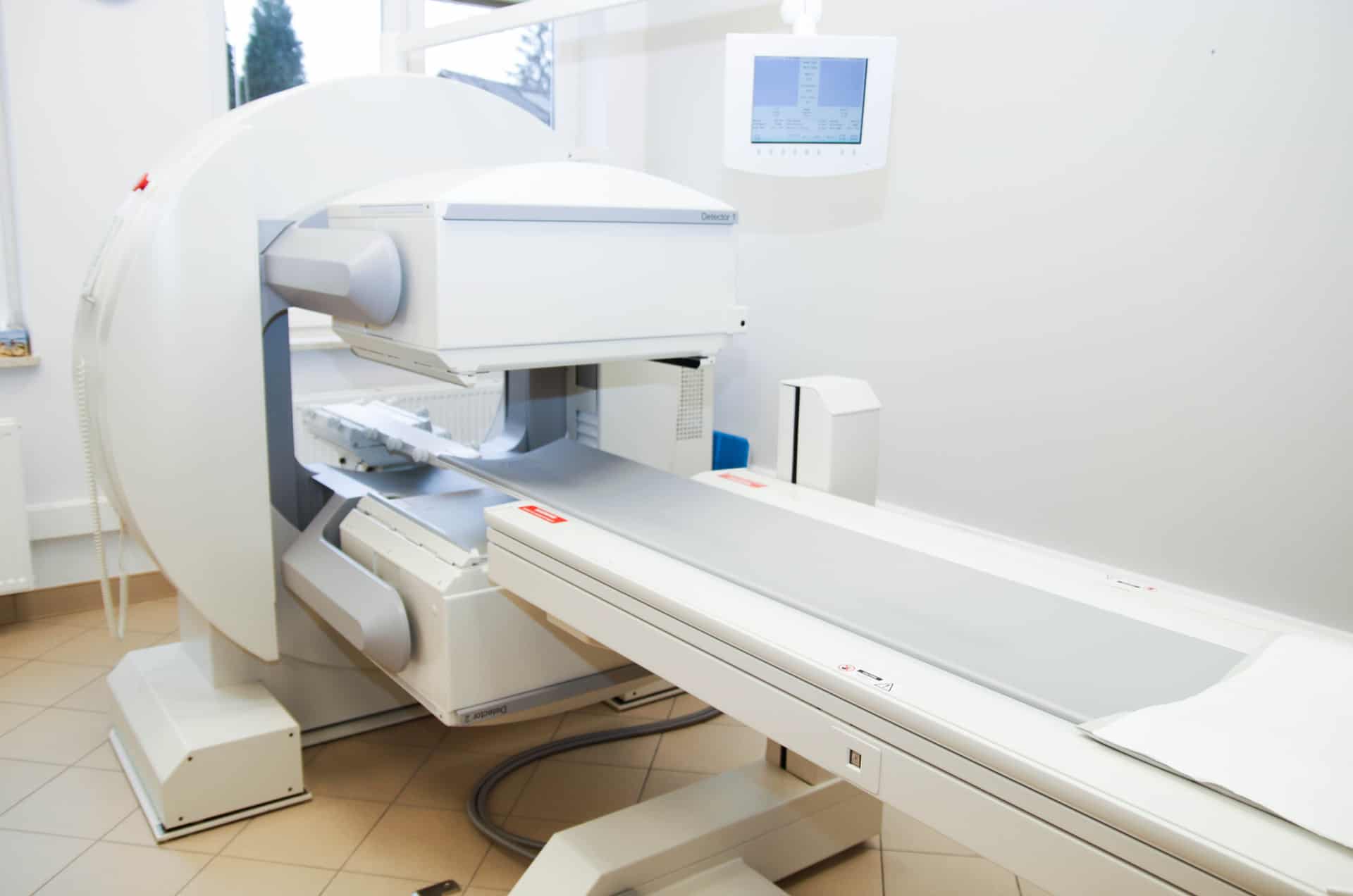
Somatostatin receptor scintigraphy
(SRS, octreotide scan, nuclear imaging of neuroendocrine tumors, NET detection)
Somatostatin receptor scintigraphy (SRS) is a nuclear imaging technique used to locate and stage neuroendocrine tumors (NETs), as well as detect metastases and/or early tumor recurrence.
SRS is currently a standard imaging modality indicated for NET staging, invaluable both in terms of choice of the best treatment option (surgery, hormonal treatment, chemotherapy, radionuclide therapy) and treatment follow-up. This study is particularly recommended in patients with NETs, who will later undergo radionuclide therapy with labelled somatostatin analogues.
The study makes use of Tc-99m radiopharmaceutical (isotopic tracer). This isotope has low gamma radiation energy and a short half-life (about 6 h), and thus is absolutely safe. Radiation load received by the patient due to SRS is lower than the one received due to many conventional radiological imaging procedures, e.g. CT of the abdomen. Somatostatin receptor scintigraphy can be offered to patients of any age and be repeated multiple times, as clinically indicated.
Different somatostatin receptor subtypes are present on the surface of the neuroendocrine tumor cells. All in all, there are five subtypes: SST1, SST2, SST3, SST4 and SST5, the most common among them being SST2 and SST5. Particles of theTc-99m based somatostatin analogue radiopharmaceuticals (e.g. Tektrotide, HYNIC-TATE, Neo-SPECT) attach themselves to these receptors, due to which even small primary tumors and metastases can be visualized in the whole-body and SPECT scintigraphic images. Somatostatin receptor scintigraphy is also a valuable diagnostic tool for detection of early tumor recurrence.
How should I prepare for the scan?
-
Stop taking somatostatin analogue drugs:
- long-acting drugs (e.g. Sandostatin LAR, Somatuline Autogel) at least 5 weeks before the scan
- short-lived drugs (e.g. Sandostatin, Somatostatin-Eumedica) at least 48 h before the scan -
Bowel voiding is recommended before the scan:
- the patient should abstain from food for at least 6 h before the scan
- easily digested food and ample fluid intake are recommended on the day before the scan
- stone fruits (plums, cherries, sweet cherries, grapes etc.) should be excluded 2-3 days before the scan
- the patient should take laxative on the day before the scan. The following laxatives can be used: Fortrans, Moviprep, Citrafleet, Eziclen (available on prescription from the referring or family doctor) -
Please bring all your previous medical records to the appointment with you:
- blood test results, hospital treatment records, histopathological test results
- medical imaging records, such as:
• computed tomography (CT) and/or magnetic resonance imaging (MRI) records incl. images saved on the CD or DVD
• ultrasound results
• positron emission tomography (PET) results
Precise detection of the pathologic changes localization and accurate interpretation of the scintigraphy results are achieved using the software-based fusion of the CT/MRI and SPECT images.
Pregnancy and breast feeding.
How is the scan performed?
- The patient checks in at the reception and hands in all their previous medical imaging records, including CD and/or DVD with the latest CT images. The patient receives an intravenous injection of the 99mTc-Tektrotide isotopic tracer. Scintigraphic images are recorded 1-4 h after the isotope administration. The patient can drink water but cannot eat during this time. The study is performed in the supine position and consists of two parts: Whole body scan is performed first, it usually takes 20 to 30 minutes. Then SPECT scans of two or three areas of interest (e.g. chest and abdomen) are carried out, each SPECT session taking about 20 minutes, depending on the localization and type of the pathologic change.
What do I need to do after the scan?
- void contact with children and pregnant women for 24 h,
- increase fluid intake to speed up tracer elimination,
- f the renal scan was performed on a baby: please remove the baby’s diaper containing radioactive urine before returning home and leave it in the clinic bathroom.